Endodontic Topics 2003, 6, 3–28
Printed in Denmark. All rights reserved
Copyright © Blackwell Munksgaard
ENDODONTIC TOPICS 2003
Life as an endodontic pathogen
Ecological differences between the untreated and root-filled root canals
GÖRAN SUNDQVIST & DAVID FIGDOR
This review describes the type of microbial flora in the untreated root canal and the root-filled canal with persistent infection. Recent contributions of molecular methods of microbial identification are outlined along with a discussion of advantages and limitations of these methods. Ecological and environmental factors are the prime reasons for differences in the microbial flora in these distinct habitats. Shared phenotypic traits and an ability to respond to the modified environment select for the species that establish a persistent root canal infection.
Introduction
Life is not easy for an endodontic pathogen. Microbes seeking to establish in the root canal must leave the nutritionally rich and diverse environment of the oral cavity, breach enamel, invade dentine, overwhelm the immune response of the pulp and settle in the remaining necrotic tissue within the root canal. During that time they have to compete in a limited space with other microbes for the available nutrition. It is no accident that microbes berth in a particular environment – there are ecological advantages for them to establish and flourish if conditions are favorable. Through genetic exchange and mutation, microbes have developed specialized systems that facilitate their ability to find, compete and survive in these very specific environments.
Bacteria are everywhere, but the environment selects
In the oral cavity, there are an estimated 1010 bacteria (1) consisting of more than 500 different kinds of microorganisms (2, 3) and all seek a niche and nutrition. One of the primary functions of tooth enamel is to exclude these microorganisms from the underlying dentine–pulp complex. As long as the enamel and cementum layers are intact, the pulp and root canal are protected from invasion, but loss of these structures by caries, cracks or trauma opens an avenue for penetration of bacteria through the dentinal tubules. All bacteria within the oral cavity share the same opportunities for invading the root canal space; however only a restricted group of species have been identified in infected root canals (4–7). The reason for the disproportionate ratio between potential and actual number of species is that the root canal is a unique environment where biological selection drives the type and course of infection. An anaerobic milieu, interactions between microbial factors and the availability of nutrition are principal elements that define the composition of the microbial flora.
In the initial phase of a root canal infection, the number of species is usually low. If the way of invasion is via caries, the bacteria in the front of the carious process are the first to reach the pulp. In cases where there is no apparent communication with the oral cavity and the bacteria penetrate through dentinal tubules, as in trauma cases without pulp exposure, there is no clear pattern of primary bacterial invaders (4, 5). The number of bacterial species in an infected root canal may vary from one to more than 12, and the number of bacterial cells varies from <102 to>108 per sample. A correlation seems to exist between the size of the periapical lesion and the number of bacterial species and cells in the root canal. Teeth with long-standing infections and large lesions usually harbor more bacterial species and have a higher density of bacteria in their root canals than teeth with small lesions.
The oral and root canal flora
Most of the resident oral microbial flora is consistent with dental health. The predominant microbial diseases of the oral cavity, caries and periodontal disease, develop at sites where a microbial biofilm, plaque, is already established and disease occurs with a change in the environmental conditions, the type and mix of microbial flora. Thus, changes at the tooth surface with a buildup of acidogenic or aciduric bacteria result in demineralization at the tooth surface, leading to caries. An increase in proteolytic bacteria at the gingival crevice is one of a sequence of factors leading to the development of periodontal disease (8). Of the major dental diseases, infection of the root canal is unique for the oral cavity since infection establishes where no microorganisms have previously been present.
The root canal as a unique site of infection
In 1894, WD Miller published his findings on the bacteriological investigation of pulps (9). He observed many different microorganisms in the infected pulp space and realized that some were uncultivable when compared with the full range observed by microscopy, and that the flora was different in the coronal, middle and apical parts of the canal system. Due to limitations of his sampling and cultivation technique, Miller was unable to verify this observation and it was not until 1982 that this could be shown by culturing (10). Differences in availability of nutrients and oxygen tension in the apical region compared with the main root canal are important reasons for the dominance of slow growing, obligately anaerobic bacteria in the apical region.
Studies on the dynamics of root canal infections have shown that the relative proportions of anaerobic microorganisms and bacterial cells increase with time and that the facultatively anaerobic bacteria are outnumbered when the canals have been infected for 3 months or more (10). When a combination of bacterial strains originally isolated from an infected root canal were inoculated in equal quantities into further canals in experimental infections, the original proportion of bacterial strains was reproduced and anaerobic bacteria dominated again (11). This illustrates that interactive mechanisms operate amongst these microorganisms, a concept further supported by the finding that when Prevotella oralis (formerly Bacteroides oralis) was inoculated on its own it was unable to survive, whereas when inoculated with other bacteria it survived and dominated the established flora (11). These experiments have shown that the endodontic milieu is a selective habitat that supports the development of specific proportions of the anaerobic microflora. Oxygen and oxygen products play an important role as ecological determinants in the development of specific proportions of the root canal microflora (12–14). The consumption of oxygen and production of carbon dioxide and hydrogen along with the development of a low reduction–oxidation potential by the early colonizers favor the growth of anaerobic bacteria.
Nutrition as an ecological driver
The type and availability of nutrients is important in establishing microbial growth. Nutrients may be derived from the oral cavity, degenerating connective tissue (13), dentinal tubule contents, or a serum-like fluid from periapical tissue (15). These factors in the root canal environment permit the growth of anaerobic bacteria capable of fermenting amino acids and peptides, whereas bacteria that primarily obtain energy by fermenting carbohydrates may be restricted by lack of available nutrients. This is the likely reason why the flora is dominated by facultatively anaerobic bacteria, such as streptococci, in the coronal section of root canals exposed to the oral cavity, and anaerobic bacteria dominate in the apical section (9, 10).
The succession of strict over facultative anaerobes with time (10, 11) is most likely due to changes in available nutrition, as well as a decrease in oxygen availability. Facultatively anaerobic bacteria grow well in anaerobiosis; however, their prime energy source is carbohydrates. A decrease in availability of carbohydrates in the root canal occurs when there is no direct communication with the oral cavity, which severely limits growth opportunities for facultative anaerobes.
The experiments of ter Steeg and van der Hoeven (16) offer important clues about the likely dynamics of the root canal flora. Using serum as a substrate, they studied the succession of subgingival plaque organisms during enrichment growth. Three phases could be distinguished during growth. Initially, rapidly growing saccharolytic bacteria consumed the low levels of carbohydrates in serum, leading to lactic and formic acid production. In a second phase, proteins were hydrolyzed, some amino acid fermentation took place, and there was digestion of remaining carbohydrates. Carbohydrates were split off from the serum glycoproteins. Growth during this phase was dominated by Prevotella intermedia, Veillonella parvula, Fusobacterium nucleatum and Eubacterium species. In a final phase, there was progressive protein degradation. The predominant species during this phase were Peptostreptococcus micros, F. nucleatum, and eubacteria. The dominance of P. micros in cultures originating from subgingival microbiota, when grown in serum, has also been shown in another study (17). The ecological niche of P. micros may be related to its wide range of peptidase activities, making amino acids and peptides available from serum glycoproteins (16). These amino acids can be used by P. micros, but also by other bacteria that have little or no proteolytic activity in serum.
The black-pigmented anaerobic rods, Prevotella intermedia/nigrescens, Porphyromonas gingivalis and Porphyromonas endodontalis, are proficient in degrading serum proteins and make peptides and amino acids available for fermentation (18). The degradation of native proteins by Prevotella and Porphyromonas species enables the growth of bacteria that depend on the availability of peptides, such as eubacteria, fusobacteria and peptostreptococci, which produce peptidases but cannot hydrolyze intact proteins (19, 20). This is also of importance for the capacity of root canal bacteria to induce periapical abscesses. Combinations of P. micros with P. intermedia or P. endodontalis have been implicated in the induction of periapical abscesses (21). Abscesses harboring a microflora that rapidly degrade serum proteins have been shown to be nearly three times larger than abscesses with a microflora that lack the capacity for breakdown of serum proteins (22).
Growth of mixed bacterial populations may depend on a food chain in which the metabolism of one species supplies essential nutrients for the growth of other members of the population (19, 23–26). Black-pigmented anaerobic rods (Prevotella and Porphyromonas species) are examples of bacteria that have very specific nutritional requirements. They are dependent on vitamin K and hemin for growth. Vitamin K can be produced by other bacteria (27). Hemin becomes available when hemoglobin is broken down, but some bacteria may also produce hemin. Another example is Campylobacter rectus which can stimulate the growth of Porphyromonas species by producing a growth factor related to hemin (26). C. rectus itself derives a source of energy from the co-inhabiting microbial species. It is strictly dependent on a respiratory mechanism in which only formate and hydrogen can serve as electron donors and fumarate, nitrate, or oxygen as electron acceptors. This makes this organism dependent on bacteria producing formate or hydrogen. A wide range of nutritional interactions is recognized among oral bacteria and these may also influence the associations between bacteria in the root canal (28–30).
Because the nutritional supply governs the dynamics of the microbial flora, it means that the bacteria present in the root canal will depend on the stage of the infection. Initially, there may be no clear associations between bacteria, but strong positive associations develop among a restricted group of the oral flora due to the type of nutrients in the environment (28, 31–33). Thus, F. nucleatum is associated with P. micros, P. endodontalis and C. rectus (28). Strong positive associations exist between P. intermedia and P. micros (28, 33) and P. anaerobius (28). There is also a positive association between P. intermedia, and P. micros, P. anaerobius and the eubacteria (28). In general, species of Eubacteria, Prevotella and Peptostreptococcus are positively associated with one another in endodontic samples (28, 31, 33). Properties that these bacteria have in common are that they ferment peptides and amino acids and are anaerobic (16), which indicates that the main source of nutrition in root canals are tissue remnants and a serum-like substrate.
Most of the species isolated from infected root canals have also been identified in the periodontal pocket (2). Although the root canal flora is not as complex as that of the periodontal pocket, they are similar in that both contain a special and limited assortment of the oral flora. It is worth noting, however, that there are some differences. When the microbial flora from root canals and periodontal pockets of non-vital teeth with periodontitis were compared (34), the ratio between anaerobic and facultatively anaerobic bacteria was approximately 100 times higher in the root canal. Anaerobic streptococci were frequent in the root canals and rarely found in the periodontal pockets. In contrast, facultative streptococci outnumbered anaerobic streptococci in the periodontal pockets. Bacteria found in root canals, but rarely in periodontal pockets were Peptostreptococcus species, Pseudoramibacter alactolyticus (formerly Eubacterium alactolyticum), P. intermedia and V. parvula. Bacteria commonly detected in periodontal pockets, but not found or found in low frequency in root canals were Prevotella melaninogenica, Prevotella corrodens and P. gingivalis.
Methods for isolation and cultivation
In order to identify microorganisms and study their characteristics and pathogenic potential, it is essential that accurate methods be used for sampling and cultivation. Microbial cells must survive the accumulated stress of sampling, dispersion, oxygen exposure, and lack of suitable nutrients in the culture media.
Anaerobic bacteriological techniques are indispensable for sampling and cultivation of endodontic bacteria. When the Virginia Polytechnic Institute (VPI) developed and simplified (35) the methods initially developed by Hungate (36), it resulted in a changed picture of the periodontal pocket flora and root canal flora. Application of these techniques to endodontic samples revealed that obligate anaerobes dominated infected root canals, comprising as much as 90% of the flora (4, 6) and confirmed the unequivocal importance of bacteria for the development of apical periodontitis in human teeth (4).
The safest way to protect anaerobic bacteria is to avoid exposure to oxygen during the various phases of the sampling and laboratory work. Oxygen is toxic because of the formation of hydrogen peroxide, superoxide radicals and hydroxyl radicals (37). The VPI method was based on achieving a low reduction–oxidation potential by gassing media with oxygen-free gas, thus affording protection from oxygenation during sterilization and subsequent handling. Another way to protect bacteria from oxygen is to use an anaerobic glove box with an atmosphere containing a mixture of nitrogen, carbon dioxide and hydrogen. Under certain conditions, anaerobic bacteria may tolerate a short exposure to oxygen (14). Media that contain hemolyzed blood have a protective effect (14). The protective effect of blood depends on the presence of the enzyme catalase, which splits hydrogen peroxide in the medium.
Because the number of bacterial cells in samples from infected root canals is so high, samples must be diluted and cultivated on solid media to allow diverse species to grow and be identified as single colonies. The dilution process is the most critical step with regard to oxygen exposure of the sample. Ideally, an anaerobic box and pre-reduced dilution solutions are used, but it can also be performed on the bench by gassing jars with oxygenfree gas. Bacteria isolated from root canals have different thresholds of sensitivity to oxygen. The most sensitive are P. anaerobius, P. endodontalis and Fusobacteria species. The rate of isolation of these species is a good indicator of how careful the measures have been to protect the sample from oxygen exposure during handling (14).
There is a correlation between the size of the periapical lesion and the number of bacterial cells and species in the root canal (4, 28). Samples taken from teeth with large, long-standing lesions harbor more bacteria (up to 108 cfu) than smaller lesions. Different colony types are most easily recognized on plates with 100 or less colonies, but additional colony types are often found on plates with up to 300 colonies. Therefore, it is reasonable to calculate that the detection level for different species is 0.3–1%. For some species, however, this level maybe lowered to 0.01% by using selective media (38).
The number of bacterial cells is dramatically reduced during root canal instrumentation and irrigation (39, 40), so for detection of bacterial cells in these samples it is necessary to inoculate solid media with undiluted samples and to use enrichment growth media, since some samples can contain less than 102 cells (41, 42). Similarly, in root canals of teeth with post-treatment disease, the number of surviving cells can be low, and all precautions must be taken to detect the bacteria. It is advisable to use as small amount as possible of sampling solution to avoid dilution of the sample, then inoculate an undiluted sample on some plates and use enrichment growth (43–45). The detection level for bacteria in teeth undergoing re-treatment depends on what bacterial species are present and on how the sample is treated, but 10–102 cells might be expected in the sample.
Cultivation discloses the broadest spectrum of the endodontic flora. When all the critical steps are well performed, cultivation allows detection of small numbers of cells in a sample. However, in samples with a high cell density the process of serial dilution means that individual species may go undetected if a species is low in number. The methods for detection of contamination, for example leaking rubber dam, or growth of bacteria under a restoration have all been based on cultivation of control samples taken after isolation, access preparation and treatment (43, 46–48).
What is an endodontic pathogen?
Over the last century, the concept of what constitutes a microbial pathogen has changed with an increasing appreciation of the complexity of the host–pathogen interaction. Recently, a revised definition has been proposed by which a pathogen is ‘a microbe capable of causing host damage’ where ‘host damage can result from either direct microbial action or the host immune response’ (49).
An endodontic pathogen is therefore defined as a microorganism capable of inducing the tissue destruction of apical periodontitis. This raises the question as to whether all microorganisms that inhabit the root canal space cause apical periodontitis, or whether specific organisms of the microbial flora are considered to cause the disease. Teeth with apical periodontitis almost always contain a polymicrobial infection and, whilst individual species may play different roles or dominate various stages of the infection, there is no evidence to suggest that particular species established therein are not involved in the pathogenesis of apical periodontitis.
Limited, but valuable information is available from a classic study (11) with an ‘eight-strain collection’ of species derived from one infected root canal that was reinoculated in equal proportions into other monkey teeth, either in toto or in various combinations of several or separate species. At the end of the experimental period, one species, Bacteroides oralis (now Prevotella oralis), dominated in mixed infections and demonstrated a more potent capacity for tissue destruction. In pure culture, however, B. oralis could not be re-isolated from inoculated root canals (11). Such findings illustrate the complexity of microbial interaction and that synergy between species may be essential for apical tissue destruction.
It is clear that much more work is needed to clarify the dynamics, functions and significance, individually and collectively, of the species constituting the root canal flora. The habitat-selected microorganisms in the infected root canal are there because of what they share in biochemical and physiological characteristics and/or what they contribute to others by mutual synergy. As far as we know today, all bacteria that establish in a root canal can be considered endodontic pathogens.
The number of microorganisms in a root canal infection is of relevance to the outcome of the disease process. Detection of just 10–50 cells of a species in a sample with 106 total cells implies a limited number of that species in the root canal and the contribution, therefore, of that number of cells to the development of disease is likely to be low. This may be a reason why studies using molecular approaches have generally failed to disclose an association between the presence of symptoms and particular species (50, 51). Molecular techniques such as polymerase-chain-reaction-based methods (PCR) do not give information on the abundance of microorganisms, whereas culturing and serial dilution provides information about the number present in a sample, and therefore what contribution they can really make to apical periodontitis. Thus, isolation and cultivation of microorganisms remain essential tools for the analysis of pathogenicity of the root canal flora.
Challenges faced by microbes establishing in the root canal
For bacteria to establish successfully as endodontic pathogens, they must overcome a series of consecutive barriers on and within the host tooth. It is likely that bacteria act in concert with others to penetrate hardand soft-tissue barriers, establish and then survive in the root canal.
The progressive challenges that microbes face in establishing in the root canal are shown in Fig. 1. In the untreated canal, microbes must breach tooth enamel by entering via microleakage, cracks or caries then reach the pulp by invading dentine. The pulp has its own host defense mechanism, which must be overwhelmed by the collective microbial consortium. Once the pulp has been invaded, the microbes must acquire suitable nutrient sources and possibly compete with others for available nutrition. The nutrition available at the tooth surface may be very different from that in pulp or in necrotic material. Finally, microbes face potential killing by the host defense. Ultimately, if successful, microbes will induce an inflammatory response at the apex resulting in apical periodontitis (Fig. 1).
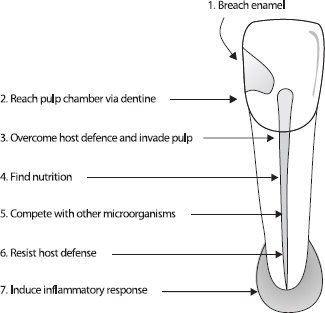
Fig. 1. Challenges for microbes to establish in the untreated root canal.
Comparison of culturing with molecular methods
Almost 40 years ago, Möller’s milestone publication (46) described how to sample the root canal in an accurate way, without contamination. The simple aim was to isolate and cultivate authentic microbial inhabitants of the root canal. With few exceptions, the papers published prior to that time had not applied the careful approach necessary for accurate isolation and cultivation. By documenting reproducible steps, recovery of microorganisms became possible without contamination from adjacent sites. The exacting principles applied to culture methods 40 years ago are no less important for recovery of microorganisms using the molecular technologies of today.
Acquiring accurate samples
Isolation of the tooth with rubber dam and decontamination of the rubber dam and tooth surface makes it possible to sample the root canal without contamination from the oral cavity (46). To check that the decontamination steps have been effective, control samples are required to ensure reliable sterility of the operative field prior to entry into the root canal (46). If the result of the control sample is positive, or in the absence of appropriate sterility checks, the veracity of the data from sampling may be in question because it is unknown whether the isolated bacteria are from within or outside the root canal.
Teeth should first be mechanically cleaned by polishing with pumice, then chemically cleaned and disinfected; before the sample is taken, the disinfectant should be inactivated so that it will not interfere with bacteria recovered from the root canal. During the access preparation, it is important to include a second decontamination stage and take a control sample before the root canal is reached, because removal of temporary fillings, carious dentin and bacteria under fillings (52) may contaminate the field (43, 46, 47). For sampling by culture, chemical cleansing with hydrogen peroxide is followed by disinfection with iodine (46).
Avoiding and managing contamination
Sampling and processing should provide a true representation of the root canal contents. When appropriate precautions are not applied, there is a risk that the results reported might not be authentic. The high sensitivity of molecular techniques, especially PCR, means that studies using these methods must use specific precautions to eliminate microbial DNA from the operation field during access preparation. When root canals are sampled by PCR, it has recently been shown that the method for decontamination requires modification (47). Cleansing with sodium hypochlorite is more efficient than hydrogen peroxide and iodine at removing detectable DNA from the tooth surface –13% of tooth surfaces were positive for detectable DNA, compared with 45%, respectively (47).
Contamination may occur not only at the site of sample recovery, but potentially during handling and laboratory procedures. The particular sensitivity of advanced culturing and molecular techniques means that many appropriate laboratory controls are necessary to avoid contamination and manage the risk. Culturing has the advantage that contamination during laboratory manipulation may be more readily recognized than with molecular procedures. PCR techniques have an inherently high risk that minute amounts of contaminating DNA are amplified and reported. There are many potential pitfalls of PCR-based analysis (53), so it is essential that the working environment is set up to reduce to a minimum the risk of contamination and that it is monitored with blank tubes, multiple positive and negative controls.
There are many procedural factors that should ensure the veracity of the results. Some examples are listed here to illustrate the kind of detailed attention necessary to deliver valid data:
- Primer design. Primers should be specific for the species and the amplified product sufficiently large. The specificity of the primers and their sensitivity should be tested and described. DNAases, released by some microorganisms at cell death, can degrade DNA in the material. The smaller fragments of DNA may persist for a longer time than larger sequences. Thus, designing the primers to target large, rather than small PCR products should yield fewer positive signals from dead cells.
- Cross-hybridization controls. There is a risk that the PCR primers designed from known 16S rRNA data may cross-hybridize with unrelated species. Therefore, controls should include checking by computer-based BLAST searches and cross-hybridization controls with live bacteria of related and unrelated species.
- Inhibition reactions. There is the possibility of inhibition reactions from constituents in the sample, which therefore require careful screening in clinical material. Collagen is one of many molecules known to be involved in inhibition reactions in clinical material.
- Optimizing PCR procedures. The optimal thermocycle parameters for PCR may differ between species. PCR conditions that are too, or insufficiently, stringent may result in poor PCR reactions with no, or wrong sequences amplified, respectively. The quality and quantity of extracted DNA depends on cell lysis conditions, which vary according to individual bacterial cell-wall structures. A low DNA recovery efficiency for some samples or some microorganisms may result in variable PCR results. For the method to be scientifically valid, it is important to verify the sensitivity and specificity of the primers.
- Sequencing the amplicon. After confirming that the amplicon is the predicted size, sequencing of the PCR product should substantiate that the amplified sequence matches that predicted from the expected species. The sequence match should be given along with the threshold for accepting identity match at species or genus levels.
Detection by PCR and culture
An important distinction needs to be made between what is evaluated by culture and PCR assays (38). Culturing measures viable bacterial cells as colony-forming units. Molecular methods measure nucleotide sequences and the PCR method allows amplification of very minute quantities of DNA to detectable levels.
Whether a root canal sample is evaluated by culturing or molecular techniques, microorganisms are acquired by the same method, usually by soaking up the fluid root canal contents with paper points. With this method, the results of laboratory processing depend on what can be recovered from the paper point. An inherent assumption in root canal sampling is that microorganisms acquired by paper point sampling reflect the type, number and diversity of the flora inhabiting the root canal. However, if the paper point does not reach all microbes, there remains a possibility that the sample may not accurately portray the root canal flora. The value and accuracy of the sample is critically dependent on how carefully the tooth is prepared, how scrupulously the sample is taken and the steps to exclude contamination. A contaminated sample is of little value regardless of whether it is later processed by molecular methods or culturing.
Culturing has the advantage that it allows all cells in a sample to grow, be subcultured and thus be identified. It has the limitation that some species have very stringent environmental and nutritional requirements that preclude culture on solid media; further, it is slow and time consuming. Culturing (and molecular methods) are highly technique sensitive and without appropriate checks may be prone to contamination and false results. Theoretically, a single bacterial cell can be detected by inoculating an undiluted root canal sample directly onto the sampling medium, but it is realistic to calculate that the limit of detection is 10–100 cells. There are two main reasons for this level of detection: serial dilution and cell survival.
Serial dilution of a sample is the primary reason for the detection limit of 10–100 cells. Serial dilution is required to:
- separate the bacteria into recognizable colonyforming units;
- reduce the numbers to 50–300 per plate for counting;
- distinguish different colony types for characterizing individual species.
During culturing some cells may die. This depends on the nutritional demands of the bacteria, how the sample is protected from oxygen exposure and on the inoculation time (54). The sensitivity of culturing can be improved with the use of selective media during subculture (38). Selective media can lower the detection limit not just because a particular species is promoted, but because other species are repressed, which then involves fewer dilutions to distinguish species.
PCR methods are well suited to target known or previously cultured and sequenced microorganisms. It can be done quickly with high specificity and where the target material is present in low amounts. PCR analysis has the advantage that it can amplify, without dilution, a particular sequence from the ambient background material. It is estimated that the DNA from 10 cells can be detected by PCR (38). Although PCR-based methods are highly specific, a disadvantage is that unidentified or non-targeted species cannot be detected, and cell numbers cannot be measured with conventional PCR. In 1996, a method that allows estimation of the number of bacteria, real-time PCR (RT-PCR), was described (55), but to our knowledge this method has not yet been applied in the analysis of endodontic infections.
Bacteria may be identified by PCR but not by culture (56, 57), although in some cases the difference is slight (58). Excluding the possibility of contamination, the likely reasons are the higher sensitivity of PCR and that PCR identifies DNA sequences, whether living or dead, compared with culturing that detects only viable cells. Whilst every living cell should be cultivable, bacteria may be undetectable by culture if (i) the number of cells is extremely low or (ii) bacteria are injured but not dead (59), (iii) the species is culture difficult (but possible) or (iv) the species is impossible to culture in vitro.
Limitations of PCR
Application of molecular methods in microbiology has revolutionized the taxonomic grouping of genera and allowed species to be systematically classified according to genetic structure rather than phenotypic behavior. The PCR technique in particular has allowed rapid identification of microorganisms that are difficult to culture. It is important, however, to recognize the limitations of this method so that interpretation of the data is reliable and valid.
The PCR method is a highly sensitive assay for DNA detection, but viable or dead cells are indistinguishable by their nucleotide sequence. Thus, microbial detection by PCR reveals current inhabitants of the root canal, but it may also represent a historical record of those microorganisms that have entered, but have not had the capacity to establish and survive. How long DNA from dead microorganisms may persist in the root canal is unknown. PCR methods have been successfully used to amplify Mycobacterium tuberculosis from several hundred to 1000-year-old animal and human remains (60–63).
The special binding affinity of hydroxyapatite for DNA has long been known (64) and this complicates recovery and analysis of the authentic endodontic microbial flora. Once DNA is adsorbed by dentine, it may prove difficult to extract (47, 65), and this problem raises several questions. For example, DNA from dead bacterial cells could be bound to coronal dentine, which could potentially contaminate the root canal sample. What is the fate of DNA from bacteria that have entered and not survived in the root canal? To date, these issues have not been adequately addressed in studies using molecular techniques, which leave open the question as to whether the reported species truly represent the living microbial flora of the root canal at the time of sampling.
There are few reports in the endodontic literature comparing results when alternative molecular methods have been applied to the same clinical material. In one study (66), checkerboard DNA–DNA hybridization was compared with 16S rDNA-based PCR. The two methods produced disparate results for the number of teeth positive for individual species and dissimilar matching between positive results. For example, Treponema denticola was detected by PCR in 23 of 50 samples and by checkerboard in five of the same 50 samples, with four samples positive by both methods. Tanerella forsythensis was positive in 11 of the 39 samples by PCR and in 15 samples by checkerboard, and only eight samples had matching positive results (66). Several factors, such as oligonucleotide design and preparation, and time/temperature protocols for hybridization and amplification could account for the disparate results.
The lack of studies with calibration of molecular methods suggests uncertainty about the authenticity and validity of reported results. Molecular methods offer sensitivity and precision, but a rigorous scientific approach with appropriate controls is essential for there to be confidence in the validity of the data.
Flora in untreated root canals
The root canal infection is a dynamic process and various bacterial species dominate at different stages of this process. In a long-standing infection, there is a shift towards dominance of the community by selected species. The most important factors driving this development are availability of nutrition, oxygen level (redox potential) and the local pH within the root canal.
Exogenous nutrients, such as fermentable carbohydrates, can affect the microbial ecology of the coronal parts of an exposed root canal, but endogenous proteins and glycoproteins are the principal nutrients in the main body of the root canal system. It might appear that the source of proteins in the root canal is restricted because of the progressive degradation of the small volume of pulpal tissue, but the bacteria induce a periapical inflammation that leads to influx of a serumlike exudate into the canal. This fluid is a sustainable nutrient source containing proteins and glycoproteins for those bacteria that have a proteolytic capacity. The bacteria that dominate this stage of the infection are likely to be those that either have a proteolytic capacity, or maintain a cooperative synergy with those that can utilize this substrate for bacterial metabolism. Bacterial metabolism of the serum-like fluid also causes reduction of the redox potential and a concomitant rise in the pH (8).
The species commonly recovered by culture from root canals of teeth with apical periodontitis have been previously reviewed (5). Application of molecular methods for microbial detection has meant that several additional species can be included as typical of the microbial flora of the infected root canal, which are described below.
Developments with molecular techniques
During the last decade, molecular techniques have increased our ability to differentiate bacteria and led to the establishment of new genera and species. To a great extent these are split off from previously established genera and species. An example of cultured bacteria that are subdivided and re-classified, are the fastidious, asaccharolytic, strict anaerobic, slow-growing, small, Gram-positive rods belonging to the genus Eubacterium. When they were first reported from root canal samples, the strains hydrolyzing arginine were characterized as Eubacterium lentum, and strains negative in this aspect were designated as ‘Eubacterium group 4’ (4). Later, strains belonging to the latter group were classified as a new species Eubacterium timidum (67). On the basis of phenotypic characteristics, DNA–DNA hybridization data and phylogenetic analysis with 16S rRNA gene sequence data, new species have been established from these two eubacteria. Oral strains of E. lentum have been re-classified as Eubacterium exiguum, later Slackia exigua (68, 69). The new genera and species Mogibacterium timidum, Mogibacterium pumilum, Mogibacterium vescum (70), Mogibacterium neglectum (71) and Cryptobacterium curtum (72) have been established from root canal and periodontal isolates of E. timidum (68).
Whilst molecular methods have helped to differentiate these species, the isolates were originally obtained by culturing from infected canals. A comparison between advanced culturing and molecular methods is possible for the species E. lentum and S. exigua, since S. exigua is the only species derived from E. lentum (68). With a species-specific PCR primer, and a detection limit of 10 organisms, S. exigua was found in 41% of teeth undergoing root canal treatment (73). This corresponds well with culturing where E. lentum has been found in 31% of teeth with necrotic pulps and periapical lesions (28). The material may not be fully comparable, but the differences in detection limits (approximately 0.5% for culture) may indicate that when this bacterium occurs, it is in numbers above this level.
Recently, studies using PCR have reported the species Dialister pneumosintes (formerly Bacteroides pneumosintes) and Filifactor alocis (formerly Fusobacterium alocis) to occur in 66% and 46% of root canals of teeth with apical periodontitis, respectively (74, 75). Because these species are non-fermentative, strictly anaerobic, slow-growing, forming diminutive colonies even after long incubation and unreactive in most biochemical tests, there are few reports of identification in culture isolates. Although D. pneumosintes was only described as a species in 1994 (76), they have been isolated by culturing (28, 77), but in lower frequencies (30–35%). The sensitivity of PCR-based screening is one obvious reason for the higher frequency of detection, but the problems involved in growth, isolation and identification are further possible reasons for infrequent identification by culture methods.
Using the PCR method, several bacterial species have been found to be more prevalent in root canals than previously reported by culture-based methods and a number of selected species are shown in Table 1.
Black-pigmented bacteria
Black-pigmented bacteria (BPB) have frequently been isolated from infected root canals and, due to their proteolytic activity, are implicated in apical abscess formation (18, 20, 21, 78, 79). P. intermedia (formerly Bacteroides intermedius) has been the most commonly isolated species. In 1992, isolates previously classified as P. intermedia were re-classified as a new species, P. nigrescens (80). P. intermedia and P. nigrescens cannot be differentiated using routine phenotypic methods. Using sodium dodecyl sulfate–polyacrylamide gel electrophoresis and PCR, it has since been shown that P. nigrescens is more common in endodontic infections than P. intermedia (81). P. intermedia and P. nigrescens have been cultured from 26–40% of root canals of teeth with apical periodontitis (28, 32, 82), although in one PCR-based study, P. intermedia/nigrescens was detected in only 13% of infected root canals (51).
Table 1. Comparison of culture (28) and molecular methods – selected species from untreated infected root canals
Prevalence (%)
| Study | F. nucleatum | Streptococcus sp.* | P. micros | P. propionicum | A. israelii | P. alactolyticus | P. intermedia/ P. nigrescens | P. gingivalis | P. endodontalis | C. rectus | F. alocis | Enterococcus sp. |
| Fouad et al. (50) | 82 | 41 | 50 | 36 | 9 | 18 | 14 | |||||
| Siqueira et al. (102) | 10 | 5 | ||||||||||
| Siqueira et al. (51) | 13 | 28 | 43 | |||||||||
| Siqueira et al. (120) | 23 | 7 | 7 | |||||||||
| Siqueira & Rôças (209) | 23 | |||||||||||
| Siqueira & Rôças (210) | 56 | |||||||||||
| Siqueira & Rôças (198) | 36 | |||||||||||
| Siqueira & Rôças (74) | 46 | |||||||||||
| Sundqvist (28) | 48 | 35 | 34 | 8 | 11 | 34 | 34 | 5 | 9 | 25 | 29 | 2 |
| *Includes facultative and stricdly anaerobic species. |
The species Prevotella tannerae has also been included in the BPB-group since strains of this species may produce tan to black pigment when grown on rabbit blood agar (83). Root canal isolates initially characterized as P. intermedia/nigrescens (84) have then been shown to be P. tannerae by 16S rRNA gene sequencing (85). Interestingly, PCR using primers specific for P. tannerae revealed that 60% of clinical isolates from root canals and abscesses/cellulitis of endodontic origin were positive for P. tannerae. Thus, P. tannerae is an example of a species that was detected in earlier culturing studies, but under a former name. The higher frequency reported in molecular compared with culturing studies is partly explained by the inconsistency of this species to form pigmented colonies (83), so that isolates may have been classified as non-pigmenting saccharolytic Prevotella species.
Of other BPB, P. endodontalis and P. gingivalis have been reported, in culture studies, to occur in frequencies lower than 10% (28, 82). In contrast, PCR assays have detected P. endodontalis and P. gingivalis in 43% and 28%, respectively, of samples from necrotic pulps (51). The sensitivity of the PCR method probably accounts for the higher reported prevalence of Porphyromonas species.
Identification of culture-difficult species with molecular techniques
Spirochetes are the group of organisms for which PCR-based identification has brought about the greatest revision of reported prevalence in endodontic infections. More than 100 years ago, some of Miller’s drawings (9) clearly indicated the presence of spirochetes. Spirochetes have then been found in necrotic root canals using microbiological methods (7, 86, 87), dark-field microscopy (88–90) and transmission electron microscopy (91). Together, these publications suggested that spirochetes were only occasionally found and when they occurred, made up a small proportion of the flora.
Recently, evidence has emerged from PCR-based analysis that infected root canals contain a range of spirochetes in much higher prevalence than was previously thought (Table 2). The most predominant spirochetes in infected root canals are T. denticola (92–94) and Treponema socranskii (92, 93). The species Treponema lecithinolyticum (95) and Treponema maltophilum (92, 95, 96) are moderately prevalent, and Treponema amylovorum (92, 95), Treponema medium (95), Treponema pectinovorum (92, 93) and Treponema vincentii (92, 93) are infrequent inhabitants of the infected root canal (Table 2).
These studies (Table 2) show considerable diversity of values between research groups, for example prevalence of T. denticola has been reported at 13% and 78% (50, 93). Even the results derived from the same research group and clinical material reveal dissimilar prevalence values, for example T. denticola is reported at 43% and 78% (93, 94). An issue yet to be resolved is whether or not a relationship exists between the presence of spirochetes and symptoms. Some findings support such a relationship (92), whereas other data suggest no association (93). Despite some progress in understanding spirochete ecology and pathogenicity (97), more information is needed to explain their role in endodontic infections.
Tanerella forsythensis (formerly Bacteroides forsythus) is an example of a bacterium that is extremely difficult to culture. This Gram-negative anaerobe is dependent on other bacteria for growth and will not grow independently in vitro, if the medium is not supplemented with N-acetyl muramic acid (98). T. forsythensis is implicated in marginal periodontitis, but to our knowledge has not been cultured from root canals. This organism was first described in infected root canals when PCR-based tests revealed evidence of it in 18% of sampled root canals (99). Using similar methods, other groups have found evidence that T. forsythensis is a relatively frequent inhabitant (Table 3), with reported prevalence values of 16–55% (50, 66, 96, 100–103).
Molecular techniques – differentiation or new species?
Molecular methods have greatly facilitated identification of culture-difficult species and expedited taxonomic grouping with ease and enhanced precision. However, the impact of molecular methods on understanding the diversity of the root canal microbiota has not been as dramatic as it might seem. With the exception of spirochetes and the species T. forsythensis, which are prevalent in infected root canals yet difficult to cultivate, molecular methods have identified species that have been previously detected by conventional culture.
Table 2. Spirochetes in infected root canals
| Prevalence (%) | ||||||||||
| Study | No. of cases (n) | T. amylovorum | T. denticota | T. lecithinolyticum | T. malthophilum | T. medium | T. pectinovorum | T. socranskii | T. vincentii | Other Treponemes |
| Baumgartner et al. (92) | 138 | 29 | 30 | 14 | 45 | 5 | 2 | |||
| Fouad et al. (50) | 24 | 13 | ||||||||
| Jung et al. (96) | 0 | 0 | 26 | 0 | 3 | 0 | ||||
| Rôças et al. (93) | 32 | 78 | 9 | 41 | 16 | |||||
| Siqueira & Rôças (95) | 31 | 7 | 26 | 39 | 13 | |||||
| Siqueira et al. (94) | 54 | 43 | ||||||||
Table 3. Tanerella forsythensis (formerly Bacteroides forsythus) in infected root canals
| Study | Number of cases (n) | Prevalence (%) |
| Fouad et al. (50) | 24 | 17 |
| Gonçalves & Mouton (100) | 11 | 55 |
| Jung et al. (96) | 73 | 16 |
| Rôças et al. (101) | 50 | 26 |
| Siqueira et al. (102) | 80 | 20 |
| Siqueira et al. (66) | 39 | 28 |
| Siqueira & Rôças (103) | 50 | 52 |
Flora in root-filled canals
It is generally acknowledged that persistence of disease is most commonly due to difficulties that occur during initial endodontic treatment. Inadequate aseptic control, poor access cavity design, missed canals, inadequate instrumentation, and leaking temporary or permanent restorations are examples of procedural pitfalls that may result in endodontic post-treatment disease (104).
The reasons for disease persistence in well-treated root-filled teeth have been poorly characterized until a series of studies published during the 1990’s. Using block biopsy material from non-healed periapical tissues including apices of the root-filled teeth, analysis by correlative light and electron microscopy has shown that there are five factors that may contribute to persistence of a periapical radiolucency after treatment. The factors are: (i) intraradicular infection (105); (ii) extraradicular infection by bacteria of the species Actinomyces israelii and Propionibacterium propionicum (106–108); (iii) foreign body reaction (109, 110); (iv) cysts, especially those containing cholesterol crystals (111); and (v) fibrous scar tissue healing (112). Of all these factors, it is generally believed that the major cause of persistent disease after root canal treatment is the persistence of microorganisms in the apical part of root-filled teeth.
Endodontic post-treatment disease, or apical periodontitis associated with a root-filled tooth, can continue for many years and may become apparent only when a tooth requires a new restoration. The fact that some microorganisms are capable of survival under harsh, nutrient-limited conditions of the root-filled canal for so long is remarkable. Yet, little information was known about the microorganisms involved in persistent intracanal infection after root filling until 1998, when two studies revealed that the microbial flora associated with endodontic post-treatment disease is quite unlike that found in other oral infections, or that of the untreated root canal (44, 45).
Microbiology of canals with persistent infection
Usually one or just a few species are recovered from canals of teeth with post-treatment disease. These are predominantly Gram-positive microorganisms and there is an equal distribution of facultative and obligate anaerobes (44, 45). This microbial flora is distinctly different from infections in untreated root canals, where the latter typically consists of a polymicrobial mix with approximately equal proportions of Grampositive and Gram-negative species, dominated by obligate anaerobes.
There is some diversity of species isolated from rootfilled teeth with persistent periapical disease, but there is a consensus amongst most studies that there is a high prevalence of enterococci and streptococci (44–46, 113–117). Other species found in higher proportions in individual studies are lactobacilli (44), Actinomyces species and peptostreptococci (116) and P. alactolyticus, P. propionicum, D. pneumosintes, and F. alocis (113). Some bacteriological findings from studies of root-filled teeth with persistent disease are shown in Table 4.
There is a difference in the microbial flora between poorly treated and well-treated teeth when the canals are sampled at re-treatment. Although only one poorly root-filled tooth was reported, the polymicrobial flora was found to be similar to that seen in untreated root canals (45). This observation has recently been confirmed in a study (117) where comparison of the isolates in 38 poorly filled canals with 22 well-filled canals revealed a significant association of the former with polymicrobial infections. When teeth are poorly treated, it is not surprising that the flora after root canal filling should approximate that of the untreated canal, especially if it is also poorly restored and there is microleakage from the oral cavity that allows an influx of carbohydrates and possibly new bacteria.
Table 4. Bacteriological findings in root filled teeth with persistent periapical lesions
| Study | Species per root canal with bacteria | Enterococcus sp.* | Streptococcus sp.* | Candida sp.* | Actinomyces sp.* |
| Möller (46) | 1.6 | 29 | 16 | 3 | ND |
| Molander et al. (44) | 1.7 | 47 | 20 | 4 | 3 |
| Sundqvist et al. (45) | 1.3 | 38 | 25 | 8 | 13 |
| Hancock et al. (116) | 1.7 | 32 | 21 | 3 | 27 |
| Peciuliene et al. (115) | 1.6 | 64 | – | 18 | – |
| Cheung & Ho (118) | 2.6(1.8)‡ | ND | 50 | 17 | ND |
| Pinheiro et al. (117) | 2.1(1.8)‡ | 55 | 33 | 4 | 20 |
| Siqueira & Rôças (113)† | 4.1 | 77 | 23 | 9 | 5 |
*Percent prevalence, in canals with microorganisms.
†Identification by PCR. All other studies by culture.
‡Excluding poorly filled root canals.
ND, not detected.
The prevalence of enterococci has been a conspicuous finding in all studies that have investigated the flora in root-filled teeth (44–46, 113–117), with one exception (118), and implicates Enterococcus faecalis as an opportunistic pathogen in persistent apical periodontitis. Streptococci are also commonly isolated from root-filled canals with persistent lesions (Table 4). Other microorganisms of interest because of their association with endodontic post-treatment disease are species of Actinomyces and Candida. Some properties of these species are described in more detail below.
Enterococci
Studies that have recovered microbes from filled root canals with persistent periapical disease have shown a high proportion of enterococci, ranging from 29% to 77% (44– 46, 113, 115–117). This contrasts with a rather low proportion of enterococci, around 5% or less, recovered from untreated infected root canals (5–7, 119, 120) and raises the question of how and when enterococci establish in the root canal. Although more research is needed to address this issue, there are several possible explanations.
One possibility is that E. faecalis could be present in untreated canals, but in such low numbers that it is not recovered, or is outcompeted by other microorganisms in the bacterial consortium. When environmental conditions improve, it may grow to higher and recoverable proportions. In animal experiments (11), after inoculation of an eight-strain collection in equal (12.5%) proportions, E. faecalis was re-isolated at about 1% of the total microbial flora, which was similar to its proportion when originally recovered from an infected tooth. Whilst this might account for some cases, it is unlikely to explain all cases since even with sensitive molecular methods, E. faecalis was only detected in 7.5% of infected root canal samples (120) compared with ten times that prevalence in canals associated with post-treatment disease (113).
There must be another explanation for the high prevalence of E. faecalis in root-filled canals associated with disease and the most likely one is that E. faecalis enters the canal in the process of treatment, during or between treatment sessions. E. faecalis has been found in a higher proportion of canals that were inadequately sealed for a period of time during the treatment, or were treated over 10 or more sessions (121). Although it is unlikely to occur when the tooth has been wellrestored, it is conceivable that E. faecalis could enter after root filling, as it has been shown that poorly restored teeth have a higher rate of endodontic posttreatment disease (122).
Enterococci are part of a stable host-adapted bacterial community inhabiting the large bowel of most adult humans in numbers as high as 108 cfu/g of feces (123). They have a commensal relationship with the host, but under favorable circumstances may take advantage of temporary weaknesses in the host defense to establish infection. The species E. faecalis has some intrinsic characteristics that allow it to survive in conditions that are commonly lethal for many other microorganisms. These properties include an ability to grow in high salt concentrations (6.5% NaCl), a wide temperature range (10–60°C), 40% bile, a broad pH range, as well as persist in the presence of detergents (124–129).
E. faecalis and Enterococcus faecium are significant human pathogens particularly in nosocomial and antibiotic-resistant infections, yet their virulence factors are just beginning to be understood (130–135). Some virulence factors identified to date (123) are: (i) secreted factors such as a cytolysin and gelatinase (136); (ii) adhesins such as aggregation substance, enterococcal surface protein (Esp), collagen adhesin (Ace) (137– 141); and (iii) surface structures such as capsular polysaccharide (142). A notable cause for concern has been the special capacity of E. faecalis for acquiring antibiotic resistance genes from other organisms or by spontaneous mutation, making it particularly difficult to control an established enterococcal infection (143).
The characteristics required for persistent infection in the root canal are unlikely to be the same as those seen in soft-tissue infection in other parts of the body. One pathogenic property is a special capacity for invasion of dentinal tubules (144–146), particularly in the presence of serum (15) and in the absence of immunoglobulin G (147). Adhesion of E. faecalis to dentine could be another factor of relevance for pathogenesis. A recent study has shown that the serine protease and a collagen-binding protein (Ace) are involved in binding E. faecalis to dentine (148).
The intrinsic capacity of E. faecalis to withstand a wide pH range represents a problem for clinical antibacterial control. Calcium hydroxide, which is generally a highly potent antimicrobial dressing (40, 149, 150), is ineffective because E. faecalis can endure a high alkalinity up to around pH 11.5 (40, 145, 146, 151–154). The natural buffering effect of dentine (155–158) affords further protection to alkaline-resistant organisms since levels in dentine do not reach higher than pH 10.8 in cervical and pH 9.7 in apical dentine (156). The mechanisms of alkaline tolerance in E. faecalis have been essentially unknown until recently when it was shown that a functioning cell-wall-associated proton pump, which drives protons into the cell to acidify the cytoplasm, is important for survival of E. faecalis in a highly alkaline environment (151). Whilst the ability of E. faecalis to resist the antimicrobial effect of calcium hydroxide remains a significant clinical challenge in endodontic re-treatment, it may not be a critical factor for its involvement in post-treatment disease. A recent study of re-treated teeth in a North American population, where calcium hydroxide is infrequently used as a root canal dressing, showed that E. faecalis was recovered in similarly high proportions (116), which suggests that resistance to calcium hydroxide may not be the explanation for selection of this microorganism.
Another inherent characteristic of enterococci is an ability to adapt to fluctuating levels of nutrient supply and limitation, and it is this trait that may facilitate the persistence of E. faecalis in the canal long after root filling. Recently, this property was explored in a series of long-term starvation assays (159). E. faecalis survived in water for more than 4 months, which demonstrated the capacity of E. faecalis to endure long-term starvation. At the onset of starvation there was a rapid fall in viable cell numbers, leaving a residual small population of starved cells (159). These starvationstate cells were shown to be in a minimal metabolic state, since addition of cell-wall and DNA synthesis inhibitors to E. faecalis starvation cultures resulted in limited change in the rate of loss of viable cell numbers.
Although there is little known about the source and type of nutrition available at the apex of a root-filled canal, the microbial flora may be sustained by a periapical tissue transudate. This is likely to be a serum-derived fluid from surrounding tissue (15, 160). Growth of E. faecalis in serum is possible (15, 161, 162). Long-term experiments with cultures of E. faecalis in human serum showed a high number of cells were still viable after 4 months (159). Cells already in a starvation state were shown to be capable of recovery upon addition of serum (159). It is likely that E. faecalis may encounter periods of starvation in the root-filled canal, broken by opportunities to access serum or serum-like fluid. Under such conditions, even a small number of cells can gain the nutritional support required for survival and would therefore have the potential to maintain a periapical disease process.
A more detailed review of enterococci and their role in post-treatment apical periodontitis appears elsewhere in this issue.
Streptococci
Streptococci comprise a relatively high proportion, approximately 20% (range 16–50%, Table 4), of the microorganisms recovered from the canals of teeth with post-treatment disease (44, 45, 115–118). However, the recovery of streptococci is less remarkable when it is taken in the context of its high prevalence in untreated infected canals (5, 32).
The genus Streptococcus contains a diverse range of species of which oral streptococci fall into four broad groups (163, 164). Analysis of the Streptococcus species isolated from teeth with endodontic post-treatment disease indicates that no particular species or group have a higher prevalence. What streptococci have in common is a preferential capacity for invasion of dentinal tubules (165–167), which should favor their ability to enter and establish in the root canal system. Streptococcal surface adhesins mediate binding to dentin as well as facilitating dentin invasion (166, 167) and streptococcal invasion of dentin may also facilitate co-invasion of other species (168).
The ability of streptococci to penetrate or hide in dentinal tubules may be attributable to their pattern of growth in chains, a phenotypic characteristic shared with enterococci. This ability may also account for the finding of streptococci in approximately the same prevalence in initial and post-treatment root canal infections.
There is some evidence suggesting that streptococci are difficult to eradicate during treatment of the root canal. In a study that evaluated bacteria before and after instrumentation of the root canals, Streptococcus species were repeatedly isolated at up to three sessions of treatment (32). Interestingly, in the same study, Candida species were also difficult to eradicate, which demonstrates the challenges faced in antimicrobial control.
Candida
Candida albicans has been periodically reported in teeth with persistent post-treatment apical periodontitis (44, 45, 113, 115–118) and yeasts have also been observed by electron microscopy in such teeth (105). Yeasts are seldom seen in untreated root canals, unless canals have been open to the oral cavity (169) or there has been a history of protracted treatment (170). In one study, the prevalence of C. albicans in infected root canals was reported to be higher, although the type of clinical material was not stated (171).
Yeasts have several properties in common with enterococci. Yeasts have the capacity to survive as a monoinfection (170, 172) and several studies have shown a capacity for growth and invasion of dentine (173–175), although in comparison with E. faecalis, this property is weak (175). Not surprisingly, sodium hypochlorite is a potent agent in killing Candida species (176–178) and EDTA is also reported to be effective (179). Several in vitro studies have reported that Candida species resist the antimicrobial action of calcium hydroxide (176, 180), which may be a factor for selection of Candida in persistent root canal infections.
These characteristics suggest that both Candida and enterococci share several properties necessary to establish and survive in the harsh environment of the rootfilled canal. The properties include resistance to antimicrobials used in endodontic treatment, an ability to grow in monoinfections, survival in conditions of nutrient limitation and an ability to evade the host response by sequestration within the root canal system.
Actinomyces
A. israelii is of interest because it is a known and repeated culprit in therapy-resistant cases (107, 181– 183) and is by far the most common species involved in actinomycosis (184). The likely site of A. israelii infection is the periapical tissues where it is known to be involved in periapical actinomycosis; however, it is interesting that it has been recovered from the root canals of re-treated teeth (45, 116, 117). The presence of A. israelii in the root canal suggests the possibility of a communication between the periapical tissues and the canal, where some protection may be afforded from the host defense.
How A. israelii establishes in the periapical tissues is unknown. It may grow out as a clump from the root canal into the periapical tissues, or it may be forced from the root canal during instrumentation, thus inoculating the periapical tissue. Studies of experimental infection with A. israelii in animals have shown characteristic lesions of a cohesive bacterial mass of branching filaments surrounded by host leukocytes (185–188).
Identification of Actinomyces species has been hampered by problems with traditional biochemical methods of characterization. Although some studies have applied DNA hybridization methods (120, 189–191), these are not readily applicable and reproducible from one lab to another. The partial characterization of the 16S rRNA gene (192) has facilitated the development of probes suited to widespread application (193–195).
A. israelii is the most prevalent Actinomyces species isolated from human abscesses; however, Actinomyces gerencseriae (formerly A. israelii serotype II) is also prevalent and they are found in 56% and 25% of human abscesses, respectively (184). Using checkerboard DNA–DNA hybridization analysis of root canal samples from teeth diagnosed with periapical abscesses, A. israelii and A. gerencseriae have been reported in 14.8% and 7.4% of samples, respectively (120); however, the role of A. gerencseriae in persistent infection after root filling is unknown.
Recently, a new Actinomyces species, Actinomyces radicidentis (196), was found to be involved in posttreatment disease (197). Using PCR-based detection, it has been shown to be present in untreated root canal infections and root-filled teeth with chronic apical periodontitis (198), although its prevalence in both types of infection was low.
Actinomyces species share some properties with enterococci, streptococci and Candida including a growth pattern of cohesive filaments or chains, resistance to antimicrobials used in endodontic treatment, an ability to grow in monoinfections and to evade the host response.
A more detailed review of Actinomyces species and their role in post-treatment apical periodontitis appears elsewhere in this issue.
Ecological differences between untreated and root-filled root canals
The untreated infected root canal is an environment that provides microorganisms with nutritional diversity in a shifting pattern over time. The species that establish have typically invaded by caries, cracks or microleakage around fillings and they seek shelter, nutrition and a favorable habitat. Initially, there may be an influx of carbohydrates facilitating growth of facultative anaerobes, but as the infection matures, the available nutrients are mainly peptides and amino acids, which favor anaerobic proteolytic species.
Whilst the microbial flora in an untreated infected root canal may experience feast, in the well-filled root canal there is predominantly famine. Most or all of the original necrotic pulp will have been eliminated leaving dry, barren conditions for surviving microbial cells. These microbes would experience a static environment and starvation, but with some luck may encounter a serum-like fluid transudate from the periapical tissue. The species that persist here are those that have either survived the antimicrobial treatment and are the last ones remaining, or have entered during treatment and found it possible to establish where others cannot do so.
Properties of species associated with endodontic post-treatment disease
With the exception of Actinomyces, which is primarily involved in extraradicular infection, other species associated with persistent intraradicular infection described here, i.e. Candida, streptococci and enterococci, can be viewed as opportunistic pathogens. A behavior in common is to leave their normal habitat of the oral cavity and establish elsewhere, in the root canal, where they take advantage of the local ecological change in the environment and where there has been elimination of microbial competitors.
For microbes to maintain apical periodontitis and cause post-treatment disease, they must do more than just survive in the root-filled canal; they must also possess the pathogenic properties necessary to perpetuate inflammation external to the root canal system. In general, microorganisms involved in persistent infections implement one of three strategies to evade the immune response – sequestration, cellular or humoral evasion (199). Sequestration involves a physical barrier between the microbe and the host. Cellular evasion means that microorganisms avoid leukocyte-dependent antibacterial mechanisms. Humoral evasion means that extracellular bacteria avoid the host’s antibodies and complement.
At least two of the three strategies are deployed by microorganisms involved in endodontic post-treatment disease (200). A. israelii is an example of an endodontic pathogen that displays cellular evasion by avoiding phagocytosis by PMN leukocytes in vivo (185, 187, 188) primarily through a mechanism of collective cohesion (188). E. faecalis and Candida species are representative of microbes that are able to remain sequestered within the root canal system.
The properties necessary for microorganisms to persist in the root-filled canal are outlined in Fig. 2. Some of the physiological traits required for entry and initial establishment may be similar to that of microbes inhabiting a necrotic pulp in an untreated canal, such as an ability to find nutrients, compete with other microorganisms and evade initial host defenses.
For species to survive endodontic treatment (Fig. 2, phase 2), there must be an ability to withstand biomechanical cleaning and antimicrobial dressing. There are numerous reports confirming the bactericidal efficacy of sodium hypochlorite against several species involved in persistent infection such as A. israelii (201), E. faecalis (151, 202, 203) and Candida (176–178). It therefore seems reasonable to assume that these species may have the capacity to shelter from the main root canal in web-like areas, or in dentinal tubules where some level of protection or buffering of the antimicrobial agent is possible (157, 204). Although most root canal bacteria are sensitive to the high pH of calcium hydroxide (40), several species involved in persistent infection are now known to have a capacity to resist the antimicrobial effect of this commonly used agent (40, 145, 146, 151, 152, 180, 201).
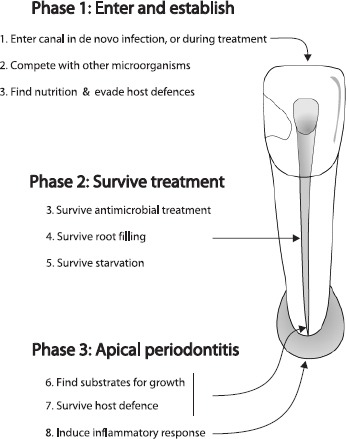
Fig. 2. Challenges for microbes involved in persistent infection.
How bacteria endure root filling is unknown, but studies that have sampled the root canal prior to root filling and then followed the treatment outcome of infected teeth have shown that some lesions heal (41, 45, 205, 206), implying that the bacteria did not survive or were not in a position to inflame the periapical tissue. Whether or not bacteria survive root canal filling may depend on whether they are entombed, or blocked from acquiring nutrition (104). It is possible, even likely, that bacteria may undergo a period of starvation. Here, the ability of E. faecalis to withstand periods of starvation (159, 207, 208), is a trait that may be crucial for survival.
Apical periodontitis is a dynamic process involving an interaction between host and living bacteria, and the microbes need to find substrates for growth (Fig. 2, phase 3). In a well-instrumented root canal where necrotic pulp tissue has been removed and there is no communication with exogenous nutrients from the oral cavity, nutrition is likely to come from a periapical fluid transudate, which is probably serum-like in nature (15). An ability to utilize collagen within dentine may also be useful and there are indications that E. faecalis may have this property (15, 148). The process of acquiring substrates for growth probably involves enzymatic breakdown of serum and tissue molecules, and this property in combination with an ability to avoid the host defense induce an inflammatory response in the periapical tissue.
Concurrent conditions for persistent infection
In a study that examined the influence of infection at the time of root filling on the outcome of treatment (41), 68% of teeth, which were infected at root filling, healed after the treatment. Similar results have also been reported in other studies (45, 205, 206). Whilst infection at the time of root canal filling will adversely affect the outcome of treatment, the presence of a persistent pathogen, alone, is not sufficient for persistence of disease. There must be a set of conditions that occur in combination to result in persistence of endodontic disease. These conditions are shown conceptually in Fig. 3. A set of microbial characteristics, coinciding with a set of location parameters permits an interaction with the host that will determine whether there will be persistent apical periodontitis.
The set of conditions for microorganisms include an ability to evade the antimicrobial stages of treatment, ‘persistence’ characteristics such as a starvation-survival potential, and a capacity to inflame host tissue (Fig. 3). Location parameters are also important. Provided that microbes can enter and reach the apical area, they must be situated near the apical (or accessory) foramen and have an open communication for the free exchange of fluid, molecules and organisms in order to inflame periapical tissue. The intersection of all these conditions with the host defense results in persistence of disease.
Fate of bacteria that have entered the root canal but do not survive
All bacteria have the theoretical capacity to enter and establish in the root canal, but few do so. Some may enter dentine, but do not reach the root canal. Others may reach the root canal, but do not survive. The fate of those bacteria that enter and reach the root canal but cannot establish or survive is unknown; however, their cell contents presumably disintegrate or are degraded by other microorganisms.
The fate of DNA from dead species is also uncertain. There remains a possibility that after lysis, the DNA fragments from these cells might linger in the canal or be bound to dentine and if so, such minute amounts would conceivably be detected and amplified by PCR. The presence of intrinsic or exogenous DNAases would also influence how long the DNA would persist.
In the only experimental study known to us that has examined the role and fate of a known microbial collection (11), various known combinations of an eight-strain collection of indigenous oral bacteria were inoculated into monkey teeth. At the end of the experimental period, Bacteroides oralis (now Prevotella oralis) dominated in mixed infections, yet could not be re-isolated when they had been inoculated in pure culture. The fate of the bacteria that were inoculated initially, but were not detected at the end of the experimental period is a matter of speculation. Whilst the species presumably died, it is also possible that some cells survived but in such low numbers that were not detectable by culture.
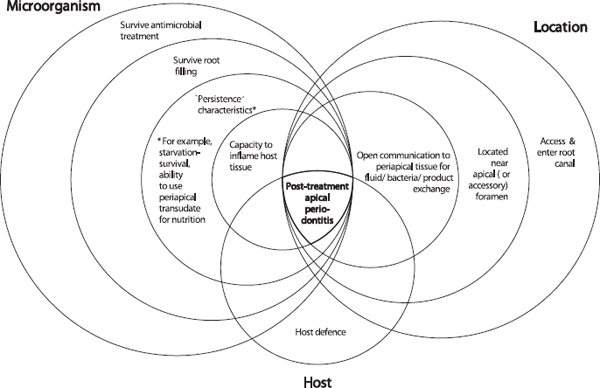
Fig. 3. Persistent infection requires not one, but a series of coupled characteristics. Bacteria must possess an ability to survive the stages of treatment, ‘persistence’ characteristics and an ultimate ability to inflame host tissue. The location of bacteria is critical for them to source nutrients and inflame tissue. The concomitant interaction of these characteristics with the host defense results in failure to heal.
In another study, subgingival plaque was grown in serum in a chemostat (16). One of the members of the microbial consortium, P. intermedia, was not detected initially, but after repeated serum enrichment it dominated the flora. This information shows that some bacteria can be present in low numbers, below the detection limit of the cultivation method.
Summary
Infection of the root canal is not a random event. The type and mix of the microbial flora develop in response to the surrounding environment. Factors that influence whether species die or survive are the particular ecological niche, nutrition, anaerobiosis, pH and competition or cooperation with other microorganisms. Species that establish a persistent root canal infection are selected by the phenotypic traits that they share in common and that are suited to the modified environment. Some of these shared characteristics include the capacity to penetrate and invade dentine, a growth pattern of chains or cohesive filaments, resistance to antimicrobials used in endodontic treatment, as well as an ability to grow in monoinfections, to survive periods of starvation and to evade the host response. Microorganisms that establish in the untreated root canal would experience an environment of nutritional diversity that changes with time. In contrast, the well-filled root canal offers the microbial flora little more than shelter from the host and microbial competitors, but in a small, dry, nutritionally limited space. In all cases, it is the environment that selects for microorganisms that possess traits suited to establishing and sustaining the disease process.